Success! TRAVEL24 has been applied to your cart.
Place your order before midnight on Monday, May 27 to receive a free travel size serum. Limited to first 500 orders.
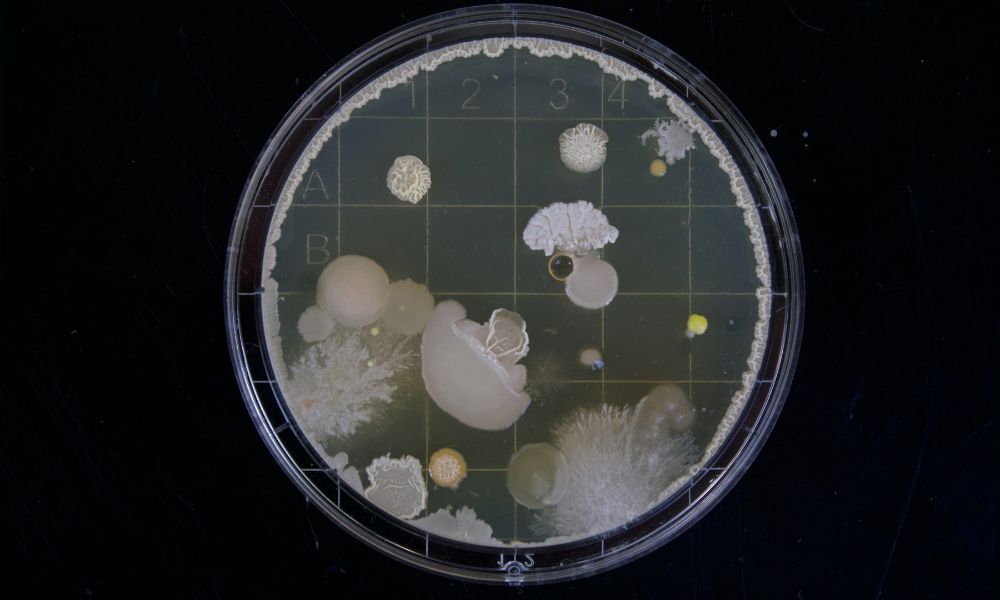
The Complete Guide to Malassezia: Causes, Biofilm, Treatment, and Prevention
Malassezia isn't a single species of fungi. Instead, the genus Malassezia refers to a group of yeasts comprising at least 17 different species, including Malassezia furfur, Malassezia globosa, and Malassezia restricta [1].
Though you may be unfamiliar with the sound of its name, this fungus is, in fact, a part of your everyday life.
It is found on everybody's skin, and it forms a part of your normal skin flora—an ecosystem of tiny organisms you won't be able to see with your naked eye.
Essentially, the Malassezia species lives on healthy skin and typically goes about its own business without stirring up too much trouble.
However, under certain circumstances, this fungus may contribute to the development of various skin infections and conditions, including pityriasis versicolor, dandruff, and seborrheic dermatitis [2].
In this article, we'll take a closer look at the Malassezia fungi and its associated skin diseases. We'll also explore what the Malassezia biofilm is and how this biofilm can be cleared.
Table of Contents:
- What Causes the Overgrowth of Malassezia?
- Common Conditions Caused by Malassezia Species
- What is the Malassezia Biofilm?
- How to Clear the Malassezia Biofilm
- Antifungals Proven to be Effective Against Malassezia
- Recommended Routine for Malassezia Overgrowth
- Final Takeaway: How to Combat the Malassezia Biofilm
What Causes the Overgrowth of Malassezia?
The proliferation (the rapid increase in population) of Malassezia yeasts on human skin is linked to various skin diseases, particularly seborrheic dermatitis.
Research has found that a flare-up of this skin disease is associated with the overgrowth of the Malassezia species [3].
While some researchers were studying Malassezia, they observed that the population of Malassezia dropped after treatment, and this occurrence was tethered to therapeutic relief and an improvement in symptoms [3].
On the other hand, they noticed that a rise in the Malassezia population was also associated with symptom relapse [3].
But what triggers or contributes to this overgrowth of Malassezia?
Well, scientists are still hard at work understanding what factors can increase the Malassezia population.
Malassezia is, in fact, lipid dependent, so it has to rely on external sources of lipids to grow and multiply.
This makes the human skin hospitable to this fungal species, as our skin glands produce an oily substance called sebum that serves as food and fuel for the Malassezia species [3].
However, seborrheic dermatitis patients may not necessarily have more sebum on their skin than those who do not have it. In other words, the level of sebum production may not be a strong risk factor for its development [3].
On the other hand, the composition of the lipids on the surface of our skin may be a factor affecting the development of seborrheic dermatitis [3].
Some research suggests that people with this skin condition may have a greater percentage of triglycerides and cholesterol on their skin surface, which may disrupt the normal balance of microorganisms present on the skin [3].
Common Conditions Caused by Malassezia Species
The Malassezia species can cause or exacerbate various skin conditions.
The following are some common skin diseases associated with Malassezia.
Seborrheic dermatitis

Seborrheic dermatitis is a skin condition characterized by inflamed skin, scaly patches, itching, flaky skin, and stubborn dandruff [4]. Seborrheic dermatitis lesions may look inflamed and sometimes present with crusting and oozing.
This skin condition commonly affects areas of your body with a high density of sebaceous glands, which secrete sebum. Areas rich in sebaceous glands include your scalp, eyebrows, eyelids, ears, the sides of your nose, and your chest [4].
Scientists have pointed out two culprits most commonly associated with seborrheic dermatitis, namely M. globosa and M. restricta.
Research has associated Malassezia with this skin condition due to several reasons [3]:
-
Seborrheic dermatitis commonly affects areas of the skin with a high density of sebaceous glands.
-
Antifungal agents, such as ketoconazole, can effectively treat the condition.
-
A flare-up of seborrheic dermatitis seems to be correlated with an increase in the population of Malassezia.
In babies and infants, seborrheic dermatitis affecting the scalp is called cradle cap. While the condition isn't serious, it can lead to crusting and yellowish or whitish scales.
Dandruff

Dandruff is the less severe version of seborrheic dermatitis and one of the most common skin conditions in the world. It affects around 50% of the population globally! [5]
Dandruff could be considered the cousin of seborrheic dermatitis, as they land on the same spectrum of disease that affects the seborrheic areas of the body [5].
This skin condition typically presents with white to yellow skin flakes that mainly affect the scalp. But the flaking could also spread to the hairline and eyebrows.
Unlike seborrheic dermatitis, dandruff does not lead to visible skin inflammation or redness [5].
Malassezia Folliculitis
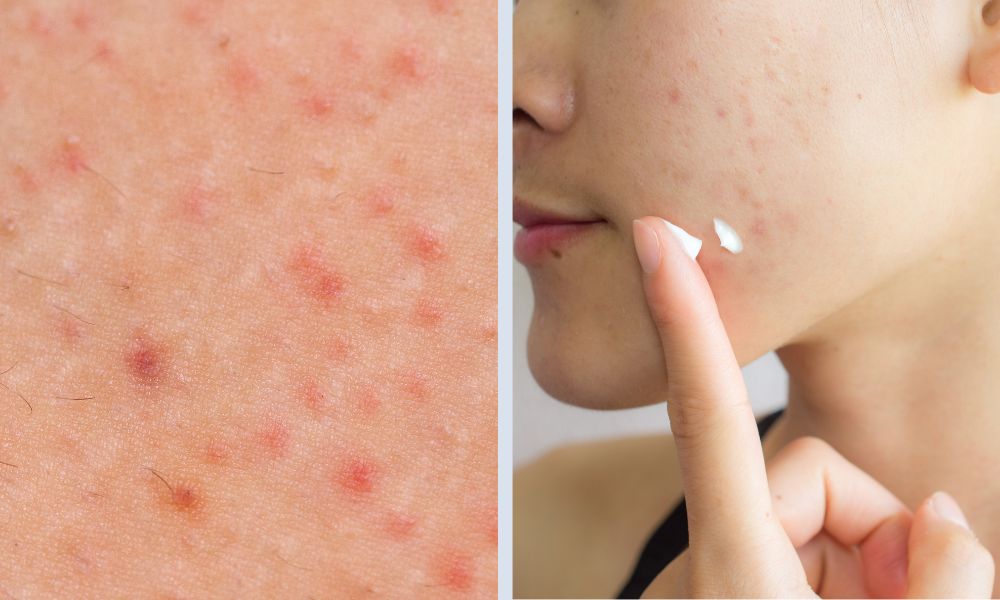
Malassezia folliculitis, also known as fungal acne, commonly presents as breakouts or pimples on your skin.
Malassezia folliculitis happens when the Malassezia yeasts infect the hair follicles on the skin, and this causes pimples to erupt on your skin's surface.
This condition resembles acne and hence, is often misdiagnosed as such. However, it is managed very differently, and your typical acne medications will not effectively manage symptoms.
The main Malassezia spp. found to be associated with fungal acne are M. globosa, M. restricta, and M. sympodialis [6].
Pityriasis Versicolor

Pityriasis versicolor, or tinea versicolor, is a common fungal infection of the skin. The predominant species of Malassezia linked to this skin infection are M. furfur, M. globosa, and M. sympodialis [7].
Malassezia fungi interfere with the skin's normal pigmentation, leading to discolored patches that usually appear on the neck, chest, arms, upper back, or tummy. These patches look scaly and, in certain cases, may be itchy [7].
Pityriasis versicolor occurs more commonly in warm and humid environments and mainly affects adolescents and young adults.
Scalp psoriasis

Though the cause of psoriasis isn't completely understood, scientists believe that this condition is linked to an issue with the immune system.
What happens is this; infection-fighting cells (immune cells) turn against your body's healthy skin cells and begin attacking them by mistake.
In response, your body begins new skin cells much faster than normal, causing these skin cells to build up rapidly on your skin's surface. This leads to scaly and pink, red, or silvery patches of skin. At times, psoriasis also involves skin itching and soreness.
Research has found that an increase in the population of Malassezia spp. may worsen scalp psoriasis in psoriasis patients [8, 9].
Atopic Dermatitis

Atopic dermatitis, also known as atopic eczema, is the most common form of eczema. Atopic eczema is a long-term, relapsing condition that causes the skin to become sore, dry, cracked, inflamed, and itchy.
Again, scientists still don't know the exact cause of this skin condition, but it is thought to be brought about by an interplay of various factors.
These include genetics, exposure to environmental triggers, and an issue with the immune system, leading to an inflammatory response and skin barrier dysfunction [10].
Some research suggests that the Malassezia species may contribute toward the development of this skin condition [11, 12].
The Malassezia fungi may interact with the skin immune system in atopic dermatitis patients, altering the release of inflammatory proteins known as cytokines.
The Malassezia yeasts can also release allergens that elicit an immune response. Because of this, Malassezia may be responsible for fuelling the development of atopic eczema in some people [11, 12].
What is the Malassezia Biofilm?

The Malassezia yeast is a lipophilic organism, meaning that it is attracted to lipids or fats. As it feeds on your skin's sebum, this yeast species will form biofilms on the skin's surface.
Scientists have been studying the antifungal susceptibility of Malassezia and whether its biofilm affects this.
In microorganisms, these biofilms act as shields and safety barriers that can increase drug resistance. Some bacteria generate their own bacterial biofilms that protect them against antibiotics.
Similarly, Malassezia species resort to forming biofilms that lead to higher antifungal resistance. Due to this, your antifungal creams, shampoos, and other topical remedies may be less effective against them [13].
How you use your medications may also affect biofilm formation. Researchers suggest that misusing antifungal agents, especially below the minimum inhibitory concentration (MIC), can enhance the fungal biofilm [13].
Hence, it is essential to consult a healthcare professional for instructions on using your prescribed antifungal medications. Unfortunately, incorrect usage of these topical agents may make the disease harder to manage in the future.
How to Clear the Malassezia Biofilm
The following are some remedies that can help disrupt the Malassezia biofilm and deactivate its protective shield.
Apple cider vinegar

Apple cider vinegar is one popular management option for seborrheic dermatitis. You can use one-part vinegar to four-parts water, though there might be a little experimentation involved to find the concentration most suitable for you.
The mixture can be applied with a cotton swab onto the affected area. Alternatively, you may use it on your scalp in the shower, together with an antifungal shampoo.
Sugar alcohols
Sugar alcohols are commonly used as natural sweeteners in foods. However, they may also help deactivate the biofilm defensive barrier that safeguards the Malassezia yeast.
Most people find that a ratio of one part sugar alcohol to four parts water works for them.
Firstly, dissolve the sugar alcohol powder in the water to form the mixture. Then, apply it to the affected regions of your skin.
Before using any of these topical DIY remedies, remember to perform a skin patch test to determine if you're allergic to any of the ingredients.
Selenium sulfide
If at-home concoctions aren't your preference, you may wish to look out for selenium sulfide, which is thought to have impressive biofilm disruption effects.
It is a chemical compound that combats itch and flakes, and you may find it in non-medicated shampoos on supermarket shelves.
High-quality colloidal silver

Another ingredient that may serve to counterattack the biofilm mechanism is colloidal silver.
Colloidal silver from a high-quality source applied to the skin is completely safe. In fact, it may help combat the itch, flaking, and inflammation associated with seborrheic dermatitis.
Lactoferrin
Lactoferrin is a protein that helps fight Malassezia and reduces the efficacy of its biofilm. Lactoferrin is more commonly found in oral supplements rather than topical products. Nonetheless, you can keep an eye out for skincare products that contain this ingredient.
The Calming Seborrheic Serum
This unique serum tackles seborrheic dermatitis from the core through a holistic approach. What it does is simple—disrupt the biofilm, clear the fungus, and soothe the skin.
Diminishing the biofilm is a crucial step, and the Calming Seborrheic Serum contains xylitol (sugar alcohol) and high-quality, third-party-tested colloidal silver to do the trick.
The all-in-one formula contains a mix of soothing ingredients to tackle itch, reduce flaking, combat inflammation, and calm the skin.
Antifungals Proven to be Effective Against Malassezia
Once the biofilm is weakened or eliminated, your antifungal agents can get to work.
We believe that combining natural remedies and lab-made methods works the best in clearing the Malassezia fungi. Of course, you can still go all-natural if that's what you're most comfortable with.
The following are some antifungal agents that can help reduce the amount of Malassezia present on your skin.
Raw Honey

One research study investigated the effects of raw honey on 30 participants who had stubborn seborrheic dermatitis.
Based on the study findings, participants who applied raw honey to the affected areas of their skin and left it on for three hours a day observed a massive improvement in their symptoms.
There was a reduction in seborrheic dermatitis skin lesions, and symptoms such as itch, scaling, and hair loss significantly improved [14].
Thus, raw honey could be an effective remedy for managing seborrheic dermatitis.
However, it will take quite a bit of commitment and discipline to slather yourself in honey and leave it on for three hours a day!
If you're up for the challenge, you can purchase medical-grade manuka honey and dilute it with water before applying it to the affected region.
You may also use a bandage or gauze to reduce mess if the application site involves your body, arms, or legs.
Garlic

Garlic has pretty impressive antifungal properties, especially when applied raw and fresh. In fact, some research suggests that garlic may inhibit the growth of Malassezia as effectively as ketoconazole (an antifungal medication) [15].
You may apply garlic directly to the affected area after mincing, juicing, or mixing it with manuka honey.
However, this remedy may not be suitable for those who dislike the smell of garlic—not to mention you probably wouldn't want to be hanging around your friends or colleagues smelling like that!
Sea salt

Salt is a compound known to have antibacterial and antifungal properties.
While there aren't many concrete studies investigating the use of sea salt specifically for Malassezia, there have been anecdotal reports of sea salt helping with seborrheic dermatitis symptoms.
If you'd like to give this natural remedy a go, you can dilute sea salt with warm (but not too hot) water. Slowly pour it over the affected area and gently massage it in. This can be left on for a few hours or overnight.
Salicylic Acid, Ketoconazole, Coal Tar, and Pyrithione Zinc

These compounds are lab-made substances used to manage seborrheic dermatitis. While these substances don't fall under the natural remedy category, we recognize that modern medicine has much to offer, too.
These medications are scientifically-backed to help reduce and control the population of Malassezia on your skin. They're effective for many people and can improve symptoms like itchy skin, scaling, and flaking [16].
Grapefruit Seed Extract

Research has reported that grapefruit seed extract has potent antifungal properties. One study found that grapefruit seed extract displayed antimicrobial effects against M. furfur and M. restricta, making it a promising ingredient for hair and skin care products [17].
Grapefruit seed extract concentrates should always be diluted before topical application to prevent skin irritation. Once diluted, you can apply the concoction once or twice daily directly to the affected regions.
Recommended Routine for Malassezia Overgrowth
A fungal skin condition typically won't go away overnight. And it'll take some consistency and patience for you to observe significant results.
But you don't need to have an extravagant or over-complicated routine in place. Having a simple yet effective routine allows you to be consistent and, in the long run, can help prevent flare-ups and recurrences.
Here are the essential steps to include in your routine.
1. Clean

Keeping the affected areas of your skin clean is one of the most simple yet crucial components of a healthy routine.
Regularly cleansing the affected regions can help clear the dead skin cells, dirt, excess oil, and fungus off your skin, which may prevent future flare-ups.
It's also best to avoid using styling products on the affected areas. For instance, hair gel and hair spray may aggravate scalp seborrheic dermatitis. Products containing alcohol may also cause the disease to flare up.
If you choose to use styling products, ensure you wash the product off thoroughly at the end of the day to reduce the chances of a flare-up.
2. Disrupt
The second step involves disrupting the Malassezia biofilm, the protective shield that keeps the fungus safe from external threats.
This biofilm can make your antifungal agents less effective, so eliminating or weakening the biofilm is also a crucial part of the recovery process.
Substances such as apple cider vinegar, selenium sulfide, and colloidal silver can help deactivate this outer shield and elevate the effects of antifungal remedies.
3. Clear
Now that the biofilm is weakened, it's time for your antifungal agents to shine.
Antifungal medications, such as ketoconazole, coal tar, and pyrithione zinc, can be purchased from your local pharmacy.
These medications come in different forms, including creams, lotions, shampoos, and ointments. Your healthcare professional can recommend the best treatment option for your case.
Of course, you can try out various natural remedies as well. Sea salt and raw honey are two substances that can help with clearing the fungus and reducing the population of Malassezia on your skin.
4. Soothe

The next step of the process involves soothing and calming the skin without feeding the fungus.
The Malassezia fungus feeds on certain types of oils. This food source supports the spread and multiplication of Malassezia—a big "no-no" if you wish to keep your symptoms under control.
The Malassezia species typically favor oils containing fatty acids with a carbon-chain length between 11 and 24. And this is the reason why oils such as olive oil and coconut oil are the top culprits on our "guilty list."
These oils are found in various haircare and skincare products. While they may help keep your skin soft, smooth, and well-hydrated, it's best not to risk fueling fungal growth by avoiding them.
On the other hand, fatty acids with a carbon-chain length between 8-10 may be harmful to the fungus and beneficial for our skin. These fatty acids include capric and caprylic acid, which can be found in MCT oil.
Apart from MCT oil, the following can also calm and soothe moody skin without fueling Malassezia growth:
-
Aloe vera
-
Urea
-
Sorbitol
-
Hyaluronic acid
-
Squalane oil
With this information in mind, go ahead and revamp your skin and scalp care routine!
How to Combat the Malassezia Biofilm
The Malassezia biofilm is a self-defense mechanism deployed by the Malassezia fungi. This biofilm can make any associated skin infection or disease more difficult to treat since the biofilm shields the fungus from antifungal agents.
Colloidal silver, lactoferrin, selenium sulfide, and apple cider vinegar can help combat the formation of this biofilm and improve the efficacy of antifungal agents.
The All-in-One Solution for Malassezia-Prone Skin
Deactivating the biofilm is just one piece of the puzzle. The Malassezia population needs to be well-controlled, and the skin requires nourishment and hydration to stay healthy.
If you're looking to combat Malassezia and restore your skin's vitality, it's best to combine different ingredients that have varying benefits.
The Calming Seborrheic Serum contains a holistic blend of ingredients with skin-soothing properties, including colloidal silver, tea tree oil, dead sea salt, and grapefruit seed extract.
Dermazen's Calming Seborrheic Serum

This serum offers much-needed relief to moody skin by reducing the itch, redness, and flaking associated with seborrheic dermatitis.
The dead sea salt, tea tree oil, grapefruit seed extract, colloidal silver, and xylitol help to reduce the population of Malassezia on the skin.
At the same time, the hyaluronic acid, MSM, urea, and concentrated aloe work to provide hydration and nourishment to the skin while calming inflammation and itchiness.